|

Today is World Hepatitis Day:
Immunisation, safe food, water - key to prevention
By Carol Aloysius
Viral hepatitis is a common water and food borne disease in Sri Lanka
following monsoon rains such as we are experiencing at present.
Among the different types of hepatitis in Sri Lanka, Hepatitis A is
the commonest as it is spread by drinking contaminated water and eating
unhygienically prepared or exposed food, such as sold on the streets or
small side cafés and restaurants.
Although this form of the disease is mild, it can still cause
discomfort to the patient and lead to complicated health risks if
neglected, affecting mainly the liver.
 Consultant Epidemiologist of the Epidemiology Unit, Ministry of
Health, Dr Manori G. Malawaraarachchi explains what the disease is and
the precautions one must take to prevent its spread in this interview
with the Sunday Observer. Consultant Epidemiologist of the Epidemiology Unit, Ministry of
Health, Dr Manori G. Malawaraarachchi explains what the disease is and
the precautions one must take to prevent its spread in this interview
with the Sunday Observer.
Excerpts …
Q. Is hepatitis a common disease in Sri Lanka?
A. Yes. Hepatitis A is a common water-borne disease found in
Sri Lanka. An average of 1,500-2,000 cases of viral hepatitis are
notified to epidemiology unit yearly. However during epidemics
(outbreaks) higher numbers (around 6000 cases) are notified.
Q. Is it endemic? Are there specific times of the year when
there are major outbreaks of the disease?
A. Yes. Viral Hepatitis is endemic in Sri Lanka and cases are
reported to the Epidemiology Unit from all 26 districts.
Sometimes outbreaks of Hepatitis A occur in some districts. Eg.
Kegalle in 2007 Kandy (Gampola) in 2009. It is possible for these
outbreaks to occur any time during a year, however they are more prone
to occur in unsanitary environments (during floods, in camps of
displaced persons etc).
Q. There are different kinds of hepatitis such as hepatitis A,
B, C. E. What kind is most common in Sri Lanka?
A. There are several types of viral hepatitis viz A B C D and
E. From these, Hepatitis A is the commonest type found in Sri Lanka.
Q. Is it caused by a virus or bacteria? How does it spread?
A. The most common causes of infective hepatitis are viruses.
There are five unrelated viruses named Hepatitis A, Hepatitis B,
Hepatitis C, Hepatitis D and Hepatitis E causing different types of
hepatitis. Hepatitis A and E are spread via faeco-oral route i.e by
ingestion of contaminated food or water. This is usually a mild disease
which has no chronic stage or a carrier state.
Transmission
Transmission of Hepatitis B, C and D occur via blood/blood products,
(during blood and blood product transfusion), body secretions (sexual
transmission) and perinatal transmission (mother to child). Blood spread
can also occur by sharing syringes in intravenous drug use, shaving
accessories such as razor blades, or touching wounds on infected
persons.
Medical personnel may contract the disease during accidental needle
prick injuries. Hepatitis B,C and D have carrier states and may progress
to chronic disease.
Symptoms
Q. What are the symptoms? How does one differentiate symptoms
of the different types of hepatitis?
A. Hepatitis A most often causes a sub-clinical or self limiting
illness. Commonly reported initial symptoms include general ill health,
loss of appetite, nausea, vomiting, head ache, mild fever. Later during
icteric phase, patients produce dark urine, pale stools and on
examination the clinician finds yellow discolouration of skin and
sclera, enlarged liver and or spleen.
 Recovery usually occurs in 3-6 weeks. In rare occasions a more severe
liver disease (fulminant hepatitis) with liver coma and death occur. Recovery usually occurs in 3-6 weeks. In rare occasions a more severe
liver disease (fulminant hepatitis) with liver coma and death occur.
Hepatitis B infection may also be sub-clinical or self limiting
(acute hepatitis) but about five percent of patients go on to become
chronic carriers of the virus. Most are ‘healthy carriers’ but some may
develop chronic active hepatitis, cirrhosis and hepato-celluler
carcinoma.With the symptoms alone one cannot differentiate the type of
hepatitis.
For an accurate diagnosis laboratory tests have to be performed. Eg.
For Hepatitis A, liver function tests and viral markers confirm the
diagnosis. The antibodies to Hepatitis A Virus IgM indicates active
infection while IgG antibodies mean immunity to disease which is common
in the general population. For Hepatitis B, laboratories will detect the
Hep B Surface Antigen (HBs).
Treatment
No treatment that can cure the disease 100 percent is available. For
mild illness no treatment is necessary. During Hepatitis A illness the
patient may be advised to rest and to follow a fat free diet and to
avoid alcohol. Strict personal hygiene and the avoidance of raw and
unpeeled foods can help prevent an infection.
Infected people excrete Hepatitis Avirus with their faeces two weeks
before and one week after the appearance of jaundice (yellow skin and
eyes).
The hepatitis B infection does not usually require treatment because
most adults clear the infection spontaneously.
Early antiviral treatment may be required in fewer than one percent
of people, whose infection takes a very aggressive course (fulminant
hepatitis) or who are with low immunity states. For chronic infection
treatment may be necessary to reduce the risk of cirrhosis and liver
cancer.
Although none of the available drugs can clear the infection, they
can stop the virus from replicating, thus minimising liver damage.
Vaccines are available to prevent Hepatitis A, and B (Hep B vaccine
also prevents Hepatitis D)
Q. What organs of the body are most affected by the disease?
A. The liver is the most affected organ. Liver cells
(hepatocytes) are lost through a gradual process of hepatocellular
injury and inflammation.
Q. What districts in Sri Lanka are usually described as
‘endemic’ to hepatitis? Why?
 A. Almost all the districts reporting Hep A cases are endemic
for the disease. However Ratnapura, Moneragala, Gampaha and Kegalle
distrcts have had high incidence over several years. A. Almost all the districts reporting Hep A cases are endemic
for the disease. However Ratnapura, Moneragala, Gampaha and Kegalle
distrcts have had high incidence over several years.
Q. What measures have been taken by the Epidemiology Unit to
prevent its spread in Sri Lanka?
A. Epidemiology Unit receives notifications of vital hepatitis
from all the districts and by analysing data it predicts outbreaks of
mainly hepatitis A and inform relevant Regional epidemiologists and
Medical Officers of Health to launch control measures prevent further
cases.
It also gives technical guidance to public health staff to control
and prevent the disease. Epidemiology Unit Unit quarterly reviews
surveillance data on viral hepatitis with Regional epidemiologists from
all 26 districts and public health experts from provinces.
The Epidemiology Unit has introduced Hepatitis B vaccines to all
infants through expanded program on immunisation since 2005. The Epid
Unit is engaged in water quality surveillance to supply safe drinking
water to the public.
The unit also regularly trains Public Health inspectors, Infection
Control Nursing Officers and other public health staff on preventing
viral hepatitis and providing safe drinking water.
Q. Is it available to the general public? Do they have to pay
for it in a government institution? What is the cost in a private
hospital?
A: Hepatitis A vaccine is not available in government sector.
Hepatitis B vaccine is provided for infants from the Government free
of charge (as pentavalent vaccine) is not provided from the Government
for general public.
Vaccines are not provided for money from the Government and high risk
medical personnel are given Hep B vaccine free of charge.
Hepatitis A and B vaccines are available in private sector.
Q. Your message to the public?
A: Viral hepatitis is a common disease in Sri Lanka. No
definite treatment is available for the disease. Prevention is the best.
Therefore to prevent the disease immunise your infants against Hepatitis
B (Pentavalent vaccine contains hep B), improve general hygiene, use
safe drinking water, consume hygienically prepared food and refrain from
risky behaviour that spread especially hep B disease.
Q. Can you give us a list of foods one should avoid eating
during floods the rainy seasons? e.g. When you say raw vegetables, do
you mean gotukola, lettuce, mallun leaves etc? How should they be eaten.
Well cooked, undercooked? How should they be washed? Will salt water
alone kill the germs or should we use something strong like turmeric
etc?
A. Washing in salt/turmeric water doesn’t kill all disease
causing organisms. In fact it may aggravate the problem if the water
used is not clean. The important thing is to wash vegetables or fruit
which are eaten raw with clean water and rinse well before consumption.
When cooking, cook well to make sure the germs are killed. Avoid food
that is eaten raw which could be contaminated with faecal matter and
consume well cooked food during flood situations.
Cover prepared/cooked food until consumption (to avoid flies/insects
contaminating food).
Q: I understand a vaccine against the disease was introduced
last year?
A: No. Hepatitis B vaccine was introduced to infants in 2003
and given island-wide since 2005 and in 2008 pentavalent vaccine was
introduced to infants which contained, Diphtheria, Pertusis, Tetanus,
Hepatitis B and Haemophylus Influnza B vaccines.
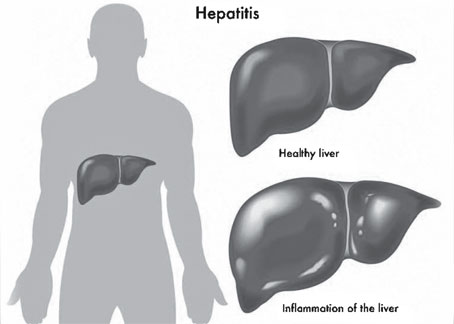
Viral hepatitis and your liver
Source: MedilinePlus
Your liver helps your body digest food, store energy and remove
poisons.
Hepatitis is a swelling of the liver that makes it stop working well.
It can lead to scarring, called cirrhosis, or to cancer.
Viruses cause most cases of hepatitis. The type of hepatitis is named
for the virus that causes it; for example, hepatitis A, hepatitis B or
hepatitis C. Drug or alcohol use can also lead to hepatitis. In other
cases, your body mistakenly attacks its own tissues. You can help
prevent some viral forms by getting a vaccine. Sometimes hepatitis goes
away by itself. If it does not, it can be treated with drugs. Sometimes
hepatitis lasts a lifetime.
Some people who have hepatitis have no symptoms. Others may have
• Loss of appetite
• Nausea and vomiting
• Diarrhea
• Dark-colored urine and pale bowel movements
• Stomach pain
• Jaundice, yellowing of skin and eyes |
Older diabetics have increased risk of physical handicap
Older adults with diabetes are at least 50 percent more likely to
have a physical disability than those without diabetes, according to the
results of a new systematic review.
Previous studies examining the risk of disability associated with
diabetes have produced varying results, ranging from no association, to
a doubling of risk. The new study is the first meta-analysis to pool
estimates taken from earlier studies, providing a more reliable estimate
of the likely risk of disability associated with diabetes.
 Led by Dr Anna Peeters and Dr Evelyn Wong, of the Baker IDI Heart and
Diabetes Institute in Melbourne, Australia, a team of researchers
examined the scientific literature to identify more than 3,000 studies
looking at the association between diabetes and disability. Led by Dr Anna Peeters and Dr Evelyn Wong, of the Baker IDI Heart and
Diabetes Institute in Melbourne, Australia, a team of researchers
examined the scientific literature to identify more than 3,000 studies
looking at the association between diabetes and disability.
The researchers then narrowed this down to eventually include 26
studies in the meta-analysis, after removing studies which were
irrelevant or not suitable for inclusion.
Disability was defined in terms of both impaired mobility, and
functional disability (impaired ability to perform activities of daily
living, such as bathing or eating, and instrumental activities of daily
living such as using the phone, shopping, and using transport).
Overall, the analysis showed that people with diabetes are at roughly
50 percent - 80 percent increased risk of physical disability, compared
to people without diabetes.
Although the study did not differentiate between Type 1 and Type 2
diabetes, the authors note that the majority of studies included in the
analysis were based on studies of older people (over 65 years), among
whom Type 2 diabetes is predominant. According to Dr Peeters, “The
reasons why diabetes is associated with physical disability are still
unclear, although several mechanisms have been suggested.
It's possible that the high blood glucose concentrations experienced
by people with diabetes might lead to chronic muscle inflammation,
eventually resulting in physical disability, and some studies have shown
that diabetes is associated with rapid and worsening muscle wasting. The
complications associated with diabetes, such as heart disease, stroke,
and kidney disease, can all result in disability.
As the world's population ages, and diabetes becomes more common, it
seems clear that we will see an increased need for disability-related
health resources, which health systems around the world need to be
prepared for.
- MNT
Inactivity, poor diet and smoking linked to disability
An unhealthy lifestyle is associated with a greater likelihood of
developing disability over the age of 65, with the risk increasing
progressively with the number of unhealthy behaviour.
 Disability is commonly defined as “difficulty or dependency in
carrying out activities essential to independent living”. With the
number of disabled people expected to increase in coming years,
researchers feel there is a need to define preventive strategies and
slow this progression. Disability is commonly defined as “difficulty or dependency in
carrying out activities essential to independent living”. With the
number of disabled people expected to increase in coming years,
researchers feel there is a need to define preventive strategies and
slow this progression.
Previous research has shown that unhealthy behaviour (such as
physical inactivity, poor diet, smoking) have an adverse effect on
health. For instance, the risk of obesity, diabetes, cancer, poor
cognitive function, stroke, sudden cardiac death and mortality increases
with the number of unhealthy behaviour.
Researchers from France and the UK therefore carried out a study to
investigate the relationship between unhealthy behaviour and the risk of
disability over a 12 year period.
They used data from the Three-City (3C) Dijon cohort study. Between
1999 and 2001, the study included community-dwelling older people (more
than 65 years old) from the city of Dijon (France); participants were
interviewed at that time about their lifestyle, including information on
smoking, diet, physical activity, and alcohol drinking. They were then
followed for the incidence of disability over 12 years.
Three levels of disability were assessed: mobility, instrumental
activities of daily living (IADL) and basic activities of daily living
(ADL). Mobility assessed the ability to do heavy work around the house,
walk half a mile, and climb stairs. IADLs included the ability to use a
telephone, manage medications and money, use public or private
transport, and do shopping, and, additionally for women, to prepare
meals and do housework and laundry.
ADLs included bathing, dressing, toileting, transferring from bed to
chair and eating. Participants were considered disabled if they could
not perform at least one activity without any given level of help.
Low or intermediate physical activity, consumption of fruit and
vegetables less than once a day, smoking (current or having quit smoking
less than 15 years ago), and no (abstention or former) or heavy
consumption of alcohol were all considered as unhealthy behaviours.
Characteristics were also identified that may influence the relation
between unhealthy behaviour and disability such as cardiovascular
disease, diabetes, depression, high BMI and cancer.
The final study included 3,982 participants of which 2,410 were women
(60.5 percent).
During the follow-up, 1,236 out of 3,982 (31 percent) participants
developed disability. The incidence of disability increased with age,
from 3.4/1000 person-years in those aged 65-70 years to 288/1000
person-years in those over 90 years of age. 922 participants died, of
whom 702 were not disabled.
Participants who developed disability were older, more likely to be
women, and less educated than participants without disability, and they
had a worse health profile.
- MNT
|


