|
Mind over matter:
A case of life and death
 Today's
column touches on an unusual subject. A story that I read last week on
the Der Spiegel Germany and Guardian UK moved me so much that I decided
to write on the issue. That is the story of Rom Houben of Belgium, who
was in a 'coma' for 23 years and was thought of only as a 'vegetable'.
Brain dead, in other words. Today's
column touches on an unusual subject. A story that I read last week on
the Der Spiegel Germany and Guardian UK moved me so much that I decided
to write on the issue. That is the story of Rom Houben of Belgium, who
was in a 'coma' for 23 years and was thought of only as a 'vegetable'.
Brain dead, in other words.
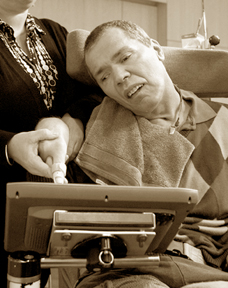 But he wasn't. The Guardian described his harrowing tale: "He saw his
doctors and nurses as they visited him during their daily rounds; he
listened to the conversations of his carers; he heard his mother deliver
the news to him that his father had died. But he could do nothing. He
was unable to communicate with his doctors or family. He could not move
his head or weep, he could only listen. But he wasn't. The Guardian described his harrowing tale: "He saw his
doctors and nurses as they visited him during their daily rounds; he
listened to the conversations of his carers; he heard his mother deliver
the news to him that his father had died. But he could do nothing. He
was unable to communicate with his doctors or family. He could not move
his head or weep, he could only listen.
Doctors presumed he was in a vegetative state following a near-fatal
car crash in 1983. They believed he could feel nothing and hear nothing.
For 23 years."
His saviour was neurologist Steven Laureys, who decided to take a
radical look at the state of diagnosed coma patients. Using a
state-of-the-art scanning system, Laureys found to his amazement that
Houben's brain was functioning almost normally.
Laureys, a neurologist at the University of Liege in Belgium,
published a study in BMC Neurology earlier this year saying Houben could
be one of many cases of falsely diagnosed comas around the world. He
discovered that although Houben was completely paralysed, he was also
completely conscious - it was just that he was unable to communicate the
fact. Houben now communicates with one finger and a special touch screen
on his wheelchair.
Laureys concluded that coma patients are misdiagnosed "on a
disturbingly regular basis". He examined 44 patients believed to be in a
vegetative state, and found that 18 of them responded to communication.
He suggests that patients suspected of being in a non-reversible coma
should be "tested 10 times" and that comas, like sleep, have different
stages and need to be monitored.
This story is slowly stirring up a hornet's nest of issues connected
with life, death, comatose states and even euthanasia. The implications
are simply too glaring to ignore. The findings are likely to reopen the
debate over when the decision should be made to terminate the lives of
those in comas who appear to be unconscious but may have almost
fully-functioning brains. Previously too, there have been reports of
coma victims who have revived and in some cases, regained full
normality.
There are many accident and stroke victims in hospitals around the
island who have suffered the same fate. They appear to be 'dead', fed by
IV and oral tubes and kept 'alive' by life support systems. Just how do
you guess that such a person could have a perfectly functioning brain ?
Doctors use an internationally-accepted scale to monitor a coma
victim's state over the years. Known as the Glasgow Coma Scale, it
requires assessment of the eyes, verbal and motor responses. But it is
still possible to miss signs that the brain is still functioning.Just
how do you deal with such a situation? That is a question that will
confront doctors, caregivers and relatives of victims worldwide in the
light of this discovery. Who has the power to decide over life ? Who can
decide that someone in a coma can no longer feel anything ? Just when do
you pull the plug out or stop feeding a comatose person ? What if he or
she is very much alive, trapped in their own body but unable to say so ?
The last time such a controversy erupted was when American Terri
Schiavo's life support was withdrawn in 2005 after 15 years in a coma.
That episode too raised many of the same questions and the medical world
itself as well as the public is still divided over the issues.
On the other hand, there are other practical and logistical issues as
well.
Is it right to keep someone in a virtually vegetative state in a
public or private hospital for years on end, whereas such facilities
could be used for a patient who could actually show signs of recovery ?
Doesn't it also prolong the agony of relatives who see a lifeless soul
who could never really be the same person again ?Again, we come to the
fundamental question of life. A coma patient is alive in the strictest
sense of the word. Doesn't pulling the plug on the life support system
or starving the person amount to killing him or her ? Just who should
decide to end a life ? Is such a life worthless ?
This also brings us to the controversial subject of euthanasia. What
if someone who is terminally ill or virtually a vegetable, but still
able to communicate slightly decides that life is no longer worth living
? A few countries do permit such patients to end their own lives with
medical assistance but in most other countries, it is considered a crime
or at least ethically unacceptable.
Proponents of euthanasia argue that terminally ill or critically
injured patients should be given the right to choose between life and
death. They say that if someone cannot ever recover from a serious
illness to lead a normal life, euthanasia could be the best way out. It
ends the pain of the patients and also the suffering of relatives, they
say.
Opponents of euthanasia note that no one, not even the patient
himself or herself, should be permitted to take a life. They say that
such a course of action amounts to plain and simple murder, even with
the patient's consent, since someone has to switch off life support
systems and/or end feeding.
What is clear is that medical science - and our minds - are far from
deciphering the fine line between life and death. We are still debating
whether a fetus can be described as a 'life' in the first few weeks. We
are still wondering whether a comatose person is alive in the strictest
sense of the word. As Houben's case amply demonstrates, we are still far
from understanding all about these vital issues. Life is a mystery,
albeit a wonderful one. Medical science and technology can help us
understand some aspects of it, but Nature is not likely to reveal all
anytime soon.
|

