|
Filaria may be deemed a scourge of the past, but...:
Danger still lurks
by Carol Aloysius
In the mid 1930s Lymphatic filariasis (LF) was one of the most
dreaded and rampant diseases in the country. Scars on untreated victims
were horrendously disfiguring causing permanent disability. Today, after
years of battling the disease with new methods of both killing the
filarial mosquito and treating the victims, Sri Lanka has successfully
brought the disease under control and eliminated it to the extent that
filaria, like many other communicable diseases that ravaged the island
in the past is now considered a disease of the past. Health officials
from the Anti- Filariasis campaign, addressing a media seminar at the
Health Education Bureau, however warned the disease could re-emerge as
small pockets of resistance had been detected in a few endemic
districts.
|

Treatment of filaria in Sri Lanka
Pic: pharmaceuticaltechnology.com |
So what does one have to watch out for? Here, Consultant Community
Physician, Anti-Filariasis Campaign, Dr S. D. Samarasekera explains the
lurking dangers, about LF, its symptoms, treatment procedures and why it
is always wise to be cautious.
Excerpts
Q:How many people are currently affected with LF worldwide?
A: Lymphatic filariasis (LF) is the fourth leading cause of
permanent and long-term disability. It is a neglected tropical disease
endemic in 83 countries, with over a billion people at risk of
infection.
Q: What are the filaria endemic areas in Sri Lanka and why?
A: In Sri Lanka, filariasis is endemic in the Western
(Colombo, Kalutara, Gampaha), Southern (Galle, Matara, Hambantota) and
the North-western (Kurunegala and Puttalam) Provinces, mainly due to
rapid and unplanned urbanization, increased population density and also
due to the suitable climate for mosquito breeding. There are Regional
Anti Filariasis Units (RAFUs) in seven endemic districts.
Q: When was the first survey on filariasis conducted in Sri
Lanka?
A: The first authentic description was found in 1936-1939: an
island-wide survey reported a microfilaria (mf) rate of 20-24% (mf
rate-percentage of persons positive for mf in night blood samples).
The Anti Filariasis Campaign (AFC) of the Ministry of Health, was
established in the Department of Health in Sri Lanka in 1947 to reduce
the burden of the disease. Two types of filarial parasites were reported
from Sri Lanka i.e. 'Wuchereria bancrofti' and 'Brugia malayi'. Since
1949 more cases of Bancroftian filariasis have been reported and there
were almost no reported cases of Brugian filariasis since 1969. At
present, 'Wuchereria bancrofti' is the main LF infection being
transmitted and few cases of Brugian filariasis have been reported.
The insect vector responsible for the spread of Bancroftian
filariasis in Sri Lanka is the female mosquitoes of Culex
quinquefasciatus.
This mosquito serves as the intermediate host and the microfilaria
count coincides with the biting habits of the vector. It breeds in
highly polluted collections of water, such as blocked drains, damaged
septic tanks, and latrine pits, which abound in urban habitats. Female
mosquitoes of Mansonia species transmit the Brugian filariasis.
Breeding of Mansonia spp. is associated with aquatic plants such as
Pistia and Salvinia.
Q: In what part of the human body does the parasite breed and
for how long?
A: The male and female adults of the filarial parasite live in
the lymphatic system of the affected person. The adults mate and produce
microfilaria (mf), which find their way to the blood stream and are
capable of living for about one year without developing further in the
human body.
When mosquito vector takes a blood meal, mf enters the mosquito from
an infected person and moults to LI, L2 and L3 larval stages of the
parasite. L3 larval stage is the infective stage where enters the human
body when a blood meal is taken by vector. Infective L3 larva converts
to adult-stage after another two months in the human body.
Q: Do all infected persons develop the disease?
A: Only a proportion of persons infected with filarial
parasites develop clinical symptoms. Lymphatic filariasis is
characterized by a wide range of clinical manifestations. The signs and
symptoms may be acute or chronic.
|
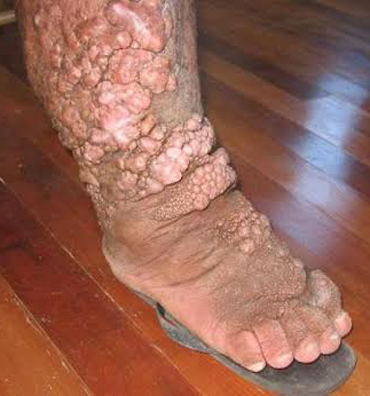
Elephantiasis-Gr4-Tuvalu
Pic: Tropicalhealthsolutions.com |
Q: What are these symptoms?
A: Patients with chronic lymphatic filariasis are usually
amicrofilaraemic (normal) and there is no currently available test to
prove active filarial infection, the diagnosis of filariasis should be
established on clinical grounds.
Acute symptoms include: fever, muscle pain, lymph node enlargement
(Lymphadenitis,) Lymphangitis, painful red patches, mild swelling of the
affected body parts. Eg: legs (more common), arms, joints (especially
knee joints and ankle joints), breasts in females, scrotum in males.
inflammatory nodules in breasts and subcutaneous tissue.
Chronic symptoms are: Hydrocele (for males), swelling of vulval area
in females, Lymphoedema, Elephantiasis, recurrent episodes of limb
lymphoedema, first pitting oedema with loss of skin elasticity and
fibrosis, are results of functional dilatation of the lymphatics. Legs
are more commonly affected than the arms.
Q: How are these patients managed?
A: Our staff routinely conducts the following activities;
parasitological surveys (through night blood filming among humans to
detect microfilaria) and treat microfilaria (mf) positive persons;
entomological surveys and vector control activities; manage lymphoedema
patients.
Q: Any advances and strategies in treatment and control of the
disease in recent years, here and abroad?
A: In 1997, following advances in diagnostics and treatment of
LF, the disease was classed as one of the six infectious diseases
considered to be 'potentially eradicable'.
The 50th World Health Assembly (WHA) adopted a resolution (WHA 50.29)
calling all member states to work towards elimination of LF as a public
health problem by 2020.
Elimination status was defined as a microfilaria rate of below 1%.
Main strategies of WHO were: (i) to stop the spread of infection
(interrupting transmission through Mass Drug Administration) -MF rate
below 1%/ Ag positivity below 2%, (2) to alleviate the suffering of
affected populations (controlling morbidity). With the support from the
international partners and the WHO, Sri Lanka successfully completed
five rounds of Mass Drug Administration (MDA) in 2006, which covered
more than 80% of the population residing in endemic eight districts in
the three provinces (Western, Southern and North Western). Two drugs
regime (DEC and Albendazole) was given during the MDA.
Q: What activities does the AFC engage in at present?
A: Conducting routine and special night blood filming
programmes in endemic areas; treating mf positive and clinically
suspected cases; managing lymphoedema patients and educating them and
their caregivers on morbidity management measures (exercise, elevation,
washing, bandaging, wearing of comfortable footwear etc.), conducting
research activities and special surveys in non-endemic areas.... We also
conduct vector surveillance and control activities in endemic areas and
hold awareness raising programmes for health staff and general public.
|
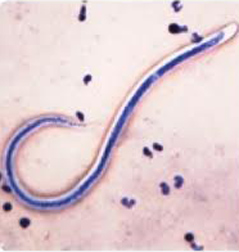
Parasitic worm-filaria |
Q: Your vision for the future?
A: To have a filariasis-free Sri Lanka; interruption of
transmission by 2020, alleviating suffering and disabilities of affected
individuals by bringing together a group of central and regional
partners to mobilize financial and technical resources to ensure
success.
Q: How will you achieve these goals?
A: By strengthening parasitological surveillance and control
activities; strengthening entomological surveillance and control
activities; strengthening laboratory facilities at AFC and regional
areas, and most importantly, preventing complications and disabilities
of affected individuals by morbidity management.
Q: Compared to a decade ago, what is the prevalence rate of
filaria in Sri Lanka today?
A: In Sri Lanka, mf rate has been below 1% over the past 10-15
years and current (2014), mf rate is 0.05%. This is very much below the
WHO elimination target.
Q: Yet despite this decline you say there are some areas that
show an increase in positive cases?
A: Even though the district data showed low mf rates, routine
and special survey data in some Medical Officer of Health (MOH) areas in
Galle District showed higher mf rate, antigen rate and mosquito
positivity. With the recommendation of the Technical Advisory Group for
National Lymphatic Filariasis Elimination Programme, Anti Filariasis
Campaign of Ministry of Health decided to give the special single dose
treatment programme in fourteen MOH areas (Akmeemana, Ambalangoda,
Balapitiya, Bope-Poddala, Elpitiya, Galle MC, Gonapinuwala, Habaraduwa,
Hikkaduwa, Rathgama, Induruwa/Bentota, Baddegama, Imaduwa and
Yakkalamulla)out of 20 MOH areas in Galle District during 2014 and 2015
considering mf positivity in the area or geographically locating closer
to a mf positive MOH area with the assistance of the Health Authorities
and Public Health Staff of the District.
The programme commenced last week and the Health staff of the MOH
will conduct it for a period of about six weeks.
Residents above two years of age in these 14 MOH will be given a
single dose of Diethylcarbamazine citrate (DEC) tablets and 400mg tablet
of albendazole. It has shown that the annual single-dose
co-administration of two drugs (DEC and albendazole) reduces blood
microfilariae by 99% for a full year.
Hence it is important to co-administer these two drugs regardless of
recent intake of anti-helminthic treatment among persons in the area.
Residents in these MOH areas are expected to consume these drugs to
control the transmission of filariasis.
The drugs will be distributed through Public Health Midwives and
Public Health Inspectors of respective MOH offices. by house to house
distribution or via drug distributing centres.
People are advised to take the drugs after meals to reduce the minor
side effects. Mass Drug Administration (MDA) is not given to: Pregnant
women, mothers breastfeeding a child below 2 years, children below 2
years and acutely ill patients.
Q: Your message?
A: The media has an important role in raising awareness on
filaria prevention activities. We appeal to you for your co-operation.. |

