|

Parkinson’s disease, treatable with early diagnosis
By Carol Aloysius
Parkinson’s disease (PD) is on the increase. Many factors have
contributed to this mostly due to increased awareness of its symptoms
and patients presenting themselves to their medical officer for early
diagnosis.
Although the bulk of the population who suffer from the disease are
elderly persons, there are a few exceptions. There are also several
myths surrounding this debilitating disease of the nervous system.
Consultant Neurologist of Anuradhapura Teaching Hospital Dr Darshana
Sirisena explains to the Sunday Observer what this disease is and how it
can be controlled.
 Excerpts… Excerpts…
Question: Parkinson’s disease now appears to be on the
increase. Your comments?
Answer: Prevalence and incidence of Parkinson's disease (PD)
has not changed overall. However the fact is that the number of patients
being diagnosed with PD is increasing. So we can assume that these
numbers may reflect a rise in the disease incidence.
This may be due to many reasons, such as patients now being more
aware of the symptoms so that seek medical advice leading to early
diagnosis. In addition at present neurological services are available
throughout the country which also contributes heavily to early and
correct diagnosis.
Q. Have you any official statistics on the number of Lankan
patients with the disease?
A. Unfortunately we have no such data with us. However, in my
experience our figures are on par with world a figure which is about 187
per 100,000 populations.
But when it applies to those above 39 years it almost doubles. Life
time risk of developing PD is about two percent and this too doubles
when a close relative is affected.
Q. Who are the people most at risk age wise and gender wise?
A. Any person can get PD but people above 60 years and males
are more at risk. (Male to female ratio is 3:2)
Q. What are the causes?
A. The vast majority of patients do not have a cause for
getting the disease. Therefore it is called as “Idiopathic Parkinson
Disease”. But in a minority of patients, genes and environmental factors
are shown to cause Parkinson's Disease.
Q. The genetic factor is still being debated on. What is your
opinion? Is the disease inherited, or only in a small proportion of
families?
A. Currently about 10 percent of newly diagnosed patients
report that someone in their family has PD which favours that genetics
play a role. At the same time twin studies have shown negative results.
So in conclusion genes do not play a major role in causing PD.
Q. Does a toxic environment contribute to the disease? If so,
what kind of toxic substances?
A. Yes, environmental interactions have contributed to the
aetiology of PD, but only in the case of a minority. MPTP (a neurotoxin)
had resulted in PD like symptoms. In addition a substance found in
pesticides (ziram) has also been implicated as an aetiological factor
for PD. Anyway, compared to the overall disease burden these factors are
negligible.
Q. Oxidative stress is said to damage the nerves. What is it?
A. Antioxidant defends and protects cells. Post-mortem studies
has shown that certain important antioxidants are lacking in PD brains
implicating oxidative stress as a pathological phenomenon in causing PD.
Simply oxidative stress, results in accumulation of certain neurotoxins
which in turn damage nerve cells ultimately causing PD. This hypothesis
needs further research.
Q. Do certain medications also trigger symptoms? Like
anti-psychotics given for treating patients with severe paranoia and
schizophrenia?
A. Yes .Certain anti-psychotic medications given for
schizophrenia and psychiatric conditions can result in Parkinsonism.
This is known as drug induced Parkinsonism. This is a common cause for
Parkinsonism and usually develops within 3 months of initiating such
medications. In addition to anti psychotics some other medications such
as certain anti-epileptic and cardiac drugs could also cause similar
symptoms.
Q. Do blood vessel disorders also lead to PD?
A. Yes. Strokes or other vascular (blood vessel disorders)
causes can mimic Parkinson like symptoms which are called as vascular
Parkinsonism. This could usually differentiate from PD clinically as
well with certain investigations such as brain imaging.
Q. What are the symptoms?
A. Classical symptoms of Parkinsonism are shaking of body
(tremor) which initially involves hands, rigidity (stiffness of the
muscles), bradykinesia (slowness of movements), and tendency to fall due
to impaired postural reflexes.
Q. How early can one detect them?
A. It is important to detect PD early as there are medications
which can control the symptoms effectively. If someone has doubts about
whether he/she or a close relative has the above symptoms, they need to
seek medical advice preferably a neurologist so can easily diagnose PD.
Parkinson's disease is entirely a clinical diagnosis as there is no
definite investigation that can diagnose PD. Investigations only help to
rule out other conditions which mimics PD.
Q. It is preventable?
A. No. It is not preventable simply because it does not have
any modifiable risk factors as Diabetes and other non communicable
diseases. But early diagnosis could lead to good quality of life.
Q. Can PD be cured? Or only controlled?
A. Parkinson's Disease could not be cured and only the
symptoms can be controlled with medications as in diabetes,
hypertension.
Q. How can it be controlled, by surgery, drugs?
A. It can be controlled largely by medications. There are many
drugs which are effective. Levodopa is the most effective out of the lot
and available freely. Important thing is how and when to initiate these
medications which is usually decided by the treating neurologist after
discussing with the patient and relatives. As the disease progresses
these medications become less effective and result in disabling
complications.
Surgical options are available but they are expensive and currently
not available in our country. In other countries surgery is usually
indicated for advanced disease patients where medications can offer only
a little.
Q. Are there new breakthroughs today like stem cell surgery to
delay the disease?
A. Though there are lots of researches currently being carried
out to find whether any process or medication could halt the disease
progression, there are no major breakthroughs so far including stem cell
surgery.
Q. What kind of care does a patient require once you get the
disease - at home?
A. In the initial stages of the disease where the symptoms are
mild and well controlled with medications patients are encouraged to be
active and mobile as much as possible and also to be function
independently as long as possible. When the disease progresses and
becomes advanced, patients are more prone to falls.
So they should work closely with the treating physician to prevent
such falls. It is also important that the patient gets a good
understanding about the disease,medications,complications and this is
mainly be possible by discussing everything with the treating physician.
Q. Are there diet restrictions?
A. No there are no special dietary restrictions but it is
important to time the medications (mainly levodopa) as the absorption is
affected by meals. Mostly patients are advised to take medications
20-30minutes before meals.
Q. How does the disease progress?
A. In most Parkinson's disease patients, the symptoms get
worse gradually over years. As the disease progresses complications will
develop which could be due to disease itself or to medications which are
disabling in most instances.
Q. What are the complications of the disease? Can it lead to
other diseases?
A. Complications are many and could be either due to disease
itself or due to medications. Commonest is that drugs become less
effective (wearing off) so that patient has to take them more often. In
addition they could develop dance like involuntary movements
(dyskinesias) which are disabling and mostly due to medications itself.
There are lots of other complications which are called non-motor
complications and they include depression, anxiety, fatigue, psychosis,
sleep disturbances, constipation, urinary retention and sensory symptoms
such as pain, numbness, restless legs etc.
Q. Can having non communicable diseases like diabetes and
cardiac problems complicate the symptoms?
A. No they are not.
Q. Any Foundation or special services available to Parkinson's
victims in Sri Lanka? If so where?
A: Unfortunately we do not have such organised, dedicated
services such as “Parkinson Support Groups” as in other countries. But
at present all major hospitals in the country have neurological services
provided by a consultant Neurologist and his team.
They can provide all the advice and services a Parkinson's patient
and his relatives need.
Q. Any other comments you wish to add?
A. Most important thing is early diagnosis and initiating
rational management depending on stage of the illness. This is only
possible by consulting a qualified physician especially a neurologist.
So if someone is doubtful of having Parkinson’s disease or already
diagnosed as having PD, the most important thing is to consult a
neurologist and clarify your doubts and learn about the illness.
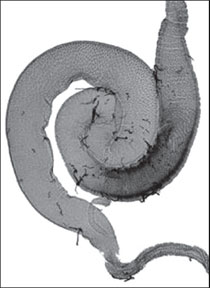
Decoding the secrets of the gut
A new technique based on atomic force microscopy was developed at the
Institute of Food Research to help ‘read’ information encoded in the gut
lining.
The lining of our gut is an important barrier between the outside
world and our bodies. Laid out, the gut lining would cover the area of a
football pitch.
 It must let nutrients from our foods through, but prevent invasion by
disease-causing bacteria, at the same time hosting the trillions of
beneficial bacteria needed for proper digestion and immune function. It must let nutrients from our foods through, but prevent invasion by
disease-causing bacteria, at the same time hosting the trillions of
beneficial bacteria needed for proper digestion and immune function.
At the forefront of the defensive system is a layer of mucus that
lines the entire gut surface. In the large bowel, the mucus layer is an
organised structure, with an inner layer that blocks bacteria, and an
outer layer where beneficial bacteria (commensals) can flourish. The
mucus layer is made up of large proteins called mucins with
characteristic sugary, or glycosylated, chains.
Dr Nathalie Juge and colleagues from the Institute of Food Research,
is leading studies aiming to understand the role of mucus in maintaining
a healthy gut and how mucins interact with bacteria in our guts.
At the molecular level, mucins exhibit clusters of glycosylation that
give the proteins a ‘bottle-brush’ appearance. The size of these
molecular sugar chains varies with location and age of the tissue, and
abnormalities in mucins are seen in inflammatory bowel diseases such as
ulcerative colitis, Crohn's disease and colon cancer.
A myriad of different conformations that the sugar chains can take up
means that mucins are incredibly diverse. The differences are believed
to help commensal bacteria by providing specific binding sites, as well
as necessary nourishment.
Pathogenic bacteria have also evolved mechanisms to bind to mucins,
as part of their arsenal to overcome our defences. We, however, are a
long way behind these bacteria in understanding the coded information
contained in these complex sugar chains.
Understanding this ‘glycocode’ would give us a new way to look at the
crucial interactions between good and bad micro-organisms in our guts,
and may also provide new insights into gut diseases.
These interactions happen at the molecular level, so for us to
understand them we need tools that work at this level. IFR has a history
of pioneering use of one such tool, atomic force microscopy (AFM). The
tip of an atomic force microscope AFM combines very high-resolution
imaging with an ability to probe the forces between molecules. AFM works
by running a very fine stylus (tip) mounted on the end of a flexible
cantilever over the surface of a molecule, much like a blind person
reading Braille.
A laser is bounced off the cantilever, amplifying the signal so that
AFM can detect distances down to a millionth the width of a sheet of
paper.
Patrick Gunning and Andrew Kirby, from IFR's AFM group, adapted this
technique by attaching sugar-binding molecules called lectins to the AFM
cantilever, via a flexible linker. They used this to probe mucins bound
to a surface. The findings of this collaborative work were published in
The FASEB Journal.
“It's a bit like fishing” said Dr Gunning. “The mucin molecules are
immersed in saline, and float like a sea of kelp. We use lectins as the
bait. We drop the line down until we hit the bottom, and then lift it
back up. If the lectin finds a target sugar molecule on the mucin, it
snags.”
Measuring the distance between the snags gives a picture of what the
overall mucin molecule looks like. By repeating this thousands of times,
and then working with IFR's biomathematicians, it was possible to
produce a ‘fingerprint’ that characterise different mucins, which means
that we could differentiate between mucins derived from different parts
of the gut.
The researchers now want to look at the mucins derived from diseased
tissues, to further investigate differences in the glycocode. They would
also like to understand how bacteria read and possibly manipulate the
glycocode. In the lab, the researchers used specific enzymes targeting
certain sugars on the mucin molecules.
This affected the mucin's molecular structure, which in turn altered
its spatial distribution. Certain bacteria in our guts also secrete
these enzymes, as a means of rewriting the glycocode for their own
benefit. With this new technique in hand, the researchers will continue
their efforts to unravel the secrets inside our own bodies.
MNT
New training package could prevent sudden cardiac death in athletes
Progress on curbing the leading killer of athletes - sudden cardiac
death - by spotting heart problems early, has been slow. But the
development of a series of online tutorials for sports and cardiology
doctors looks set to reverse this trend.
The tutorials, which are free to any doctor around the globe, thanks
to the backing of the American Medical Society for Sports Medicine
(AMSSM) and FIFA, aim to teach physicians how to read heart monitor
tracings (ECGs) and spot abnormalities linked to potentially fatal
disorders.
Some inborn heart conditions are difficult to detect, because they
progress silently, and are only diagnosed when intense exercise triggers
a lethal heart rhythm - sudden cardiac arrest.
 According to the American Heart Association, over 7000 people under
the age of 18 die every year in the US of a sudden cardiac arrest. According to the American Heart Association, over 7000 people under
the age of 18 die every year in the US of a sudden cardiac arrest.
Studies suggest the risk is three times higher in competitive
athletes. Last year in the UK, footballer Fabrice Muamba collapsed on
the pitch following a sudden cardiac arrest at the age of 24. He
received prompt expert medical attention which helped him make a
remarkable recovery.
But many athletes are not as lucky, and trying to pick up those most
at risk is the only way of warding off sudden cardiac arrest, which
could be - and often is - deadly.
And interpreting ECGs in athletes can be difficult, because their
hearts have adapted to the stress of extensive training and top level
performance.
Initiated by Professor Jonathan Drezner, AMSSM President, in
association with BMJ Learning and the British Journal of Sports
Medicine, and developed and written by international experts in sports
medicine and sports cardiology, the online tutorials guide doctors on
how to recognise ECG changes that indicate problems rather than healthy
cardiac adaptation.
“Whether used for diagnostic or screening purposes, ECG
interpretation is a fundamental skill for doctors involved in the
cardiovascular care of athletes,” said Prof Drezner.
He said, “These online learning modules provide doctors with a common
basis for interpreting an athlete's ECG, improving their chances of
making an accurate diagnosis, and of picking up potentially
life-threatening problems earlier.”
The modules draw on a series of papers presenting new consensus
standards on ECG interpretation in athletes, published in the British
Journal of Sports Medicine.
- MNT
High heart rate at rest signals higher risk of death
A high heart rate (pulse) at rest is linked to a higher risk of death
even in physically fit, healthy people, suggests research published in
the journal Heart.
A resting heart rate - the number of heart beats per minute - is
determined by an individual's level of physical fitness, circulating
hormones, and the autonomic nervous system. A rate at rest of between 60
and 100 beats per minute is considered normal.
People who are very physically active tend to have a low heart rate
at rest, but the authors wanted to find out if heart rate had any
bearing on an individual's risk of death, irrespective of their level of
cardiorespiratory fitness.
They therefore tracked the health of just under 3,000 men for 16
years, all of whom were part of the Copenhagen Male Study.
This was set up in 1970-71 to monitor the cardiovascular health of
middle aged men at 14 large companies in Copenhagen.
In 1971 all participants were interviewed by a doctor about their
health and lifestyle, including smoking and exercise, and given a
check-up.
Their cardiorespiratory fitness was assessed using a cycling test,
set at three different levels of exertion.
In 1985-6, just under 3,000 of these original participants were given
a further check-up, to include measurements of height, weight, blood
pressure, blood fats and blood glucose. Their resting heart rate was
also recorded (ECG and VO2Max). Sixteen years later in 2001, the
researchers checked national Danish registers to find out which of these
men had survived. Almost four out of 10 (39 percent; 1,082) of the men
had died by 2001.
Unsurprisingly, a high resting heart rate was associated with lower
levels of physical fitness, higher blood pressure and weight, and higher
levels of circulating blood fats. Similarly, men who were physically
active tended to have lower resting heart rates.
- Medicalxpress |


